
Background information
Can make-up harm your eyes? An interview with an optometrist
by Natalie Hemengül

Athlete’s foot is unpleasant and quite disgusting. If you have this condition, you probably won’t mention it in public. According to studies, about 25% of people will have it once in their lifetime. But it doesn’t have to be that way.
Fungi – aka mushrooms – are all the rage, have «the makings of a meat substitute», can manipulate insects and be used as a plant-based leather alternative. But sometimes fungus can cause pain and cracks or marks on the skin, which are unsightly and/or sore.
What forest and skin fungi have in common is they always prefer slightly moist and warm environments. Filamentous fungi (dermatophytes) differ from yeasts and mould.
The most common fungal condition is athlete’s foot, which falls under the filamentous fungi umbrella. Studies such as this one show that it affects approximately a quarter of the population. These fungal infections are often found between the fourth and fifth toe. They spread in damp and warm conditions and in small cracks in the skin if your feet are sweaty or wet from the pool.
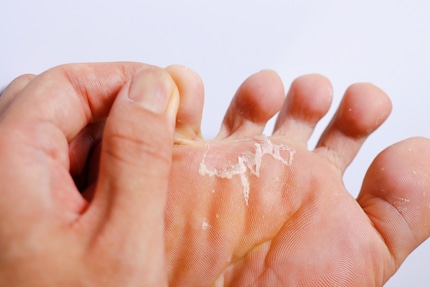
Fungal infections like this are often itchy at first, before the skin gets red and sometimes progresses into much deeper, painful cracks. Old people are plagued more often than their younger counterparts, as they have more layers of keratin. In other words, thicker calluses that the fungus can nestle between and thrive in. Athletes who constantly work out in plastic shoes – cue sweaty feet – and then use communal showers, are more likely to develop the aptly named condition called athlete’s foot. For most, it’s harmless, but still needs to be treated to stop it spreading. If the fungal infection has also reached the nails (nail fungus), it’s a lot more difficult to treat.
To avoid athlete’s foot, it helps to dry your shoes properly when they get wet. If you don’t have a hand or hair dryer and plenty of spare time on your hands, a proper shoe dryer or the good old hack of stuffing your shoes with newspaper could be worthwhile.
If you’re prone to athlete’s foot, you can take protective measures against lurking fungi on the foot bed by using antibacterial shoe sprays. Equally, always being barefoot, prevents any fungus getting a foothold. If that’s too cold for you, you’ll need to change your socks and shoes regularly, especially if they’re sweaty.
All fungi is infectious, which means there’s likely to be some lurking where there’s a lot of people going about barefoot (swimming pools, changing rooms, communal showers). If your towels and safety mats get washed at 60°C, you won’t be able to detect any fungus on them. Hand disinfectant is also as effective on feet – just be sure to let it dry. Moisturise dry, cracked skin if possible, so that fungus can’t use crevices as a breeding ground.
The symptoms of athlete’s foot are so typical that it’s hard to mistake for anything else. However, if you’re in doubt, scrape some skin flakes off the affected area, dip them in potassium hydroxide and marvel at the beautiful looking fungi under the microscope.
If the fungal infection spreads extensively, you’ll want to get your immune system checked. People with low immunity are more susceptible to fungi. Sometimes the area that only had a minor fungal infection to begin with also becomes inflamed. People who can’t feel their feet well, such as those with later-stage diabetes, often have an extensive infection because they don’t notice the pain of it spreading.
Anti-fungal creams and ointments you rub onto the skin are good remedies, despite their unpronounceable names – by me, in any case. A lot of them contain active ingredients from the group of pyridones (e.g. Ciclopirox), allylamines (e.g. Terbinafine and Naftidine) and azoles (Clotrimazole, Bifonazole, Miconazole and Oxiconazole). Most of the time, you need to apply ointment/cream or lotion twice a day for several weeks.
Header image: Shutterstock
Family and paediatrician, family counselling for big and small people. Loves emergency care and rescue transports and the interface with basic and clinical research. Journalism started with the school newspaper, later stations at the Deutsche Welle, the Deutsches Ärzteblatt, author of scientific publications.
Interesting facts about products, behind-the-scenes looks at manufacturers and deep-dives on interesting people.
Show all
Background information
by Natalie Hemengül

Background information
by Mareike Steger

Background information
by Tanja Restin